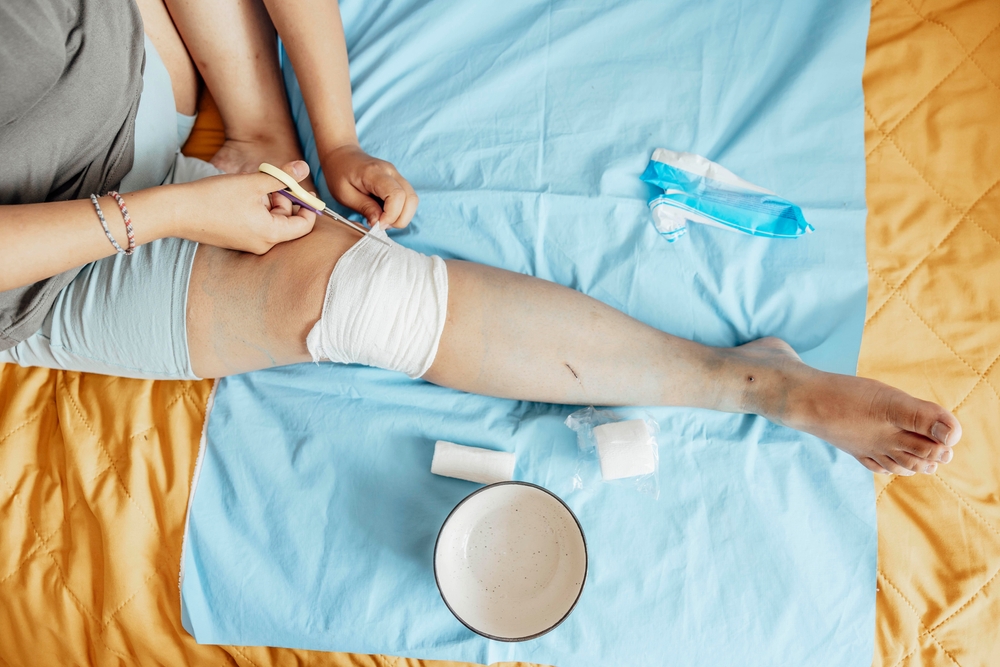
When you have a wound, it’s important to try to stop infection. If bacteria get into broken skin, your body heals more slowly, and other problems can arise, prolonging healing and increasing the risk of serious health issues.
Wound infection prevention is not complicated, but it does require careful, consistent wound care, especially in the early stages.
In this guide, the wound care specialists at Innovative Wound Care Specialists in Flint, Michigan, share useful, easy-to-understand tips for stopping wound infections and helps you know when you should see a wound care specialist for expert advice.
How Do You Prevent a Wound Infection?
To prevent a wound infection, you must be proactive from the beginning. The goal of proper wound care at home is to reduce bacterial exposure, protect the tissue, and support the body’s natural healing process.
The 5 Rules of Wound Care: Your First Line of Defense in Wound Healing
When it comes to preventing wound infections, there are basic steps that apply in most situations. That said, wounds vary in type and severity, and each may require slightly different skin care for wound healing based on depth, location, and underlying health conditions. You should always follow your provider’s specific instructions.
1. The Golden Rule: Wash Your Hands Before and After Touching the Wound
Hand hygiene is the first and most important step in preventing a wound infection.
Wash your hands with soap and warm water for at least 20 seconds before cleaning or dressing a wound. Someone helping with care should do the same. Clean hands help prevent bacteria from reaching vulnerable tissue.
2. Clean the Wound and Surrounding Skin
Always follow your specialist’s wound cleaning instructions. Typically, this includes gently rinsing the wound with clean, running water to remove dirt and debris.
Never use hydrogen peroxide, iodine, or rubbing alcohol on open wounds. These products can irritate the tissue and slow healing.
Clean the surrounding skin with sterile saline or mild soap to remove any residue, but avoid getting cleanser into the wound.
If you cannot easily rinse out visible material with water, or if the wound is deep or continues bleeding, do not continue to attempt wound cleaning at home. It should be evaluated by a medical professional.
3. Keep the Wound Moist and Covered
Wounds heal better in a slightly moist, covered setting. If exposed to air, tissue can dry out, making it more vulnerable to irritation and contamination. Keeping wounds covered supports the body’s healing process.
Wounds should be covered with a sterile bandage or dressing suited to the wound’s size and depth. If your healthcare provider has recommended a topical product, you will apply a thin layer as directed, then cover the wound.
Petroleum jelly and some ointments help maintain moisture, which aids tissue repair and lessens scab formation that can slow healing. Use topical antibiotics only if advised.
4. Daily Dressing Maintenance
Change dressings at least daily, or sooner if wet or dirty. This keeps the wound clean and helps you watch for early signs of infection, such as increasing redness, swelling, drainage, or worsening pain.
For surgical wounds, chronic ulcers, or complex injuries, your doctor may recommend a different dressing schedule or specific products based on the wound type and your overall health. Always follow the individualized instructions provided by your healthcare professional.
5: Seek Professional Wound Care
Even with careful home care, some wounds require medical evaluation. Early evaluation can help prevent complications and support safe healing.
Call a doctor if you see worsening pain, redness spreading, warmth, swelling, drainage with odor, fever, or red streaks. Deep, bite, or non-healing wounds should be evaluated.
Additionally, if you have diabetes, vascular disease, or a weakened immune system, it’s always best to seek care earlier rather than waiting for symptoms to worsen.
Lifestyle Factors That Support Wound Healing
Cleaning and dressing wounds reduce infection risk, but internal factors matter too. Circulation, blood sugar, immune function, and diet all influence healing and resistance to infection.
Blood Sugar Management
Elevated blood sugar can impair circulation and weaken the immune response. For individuals with diabetes, maintaining stable blood glucose levels is one of the most important factors in reducing the risk of infection and supporting wound healing.
Nutrition and Hydration
Healthy eating doesn’t replace proper wound care, but it can directly influence the body’s ability to heal because tissue repair requires adequate protein and key nutrients.
Protein helps rebuild tissue, vitamin C aids collagen, and zinc supports repair. Hydration helps deliver nutrients and oxygen.
To learn more, read “Nutrition Tips for Wound Care.”
Circulation and Movement
Healthy blood flow is necessary to deliver oxygen and nutrients to damaged tissue. Reduced blood flow, especially in the lower extremities, is a common cause of delayed wound healing. Gentle daily movement appropriate for your health can support circulation and vascular function.
Avoid Tobacco Use
Smoking reduces oxygen delivery to tissues and constricts blood vessels, both of which can slow healing and increase the risk of infection. Avoiding tobacco use supports more efficient tissue repair.
The Telltale Signs of Infection: How Do You Know If a Wound Is Infected or Healing?
The key difference between a healing wound and an infected wound is the progression of the infection. Healing wounds gradually improves. Infected wounds tend to become more painful, red, irritated, or inflamed rather than improve.
It is normal for a wound to look slightly red or feel tender in the first few days. Mild swelling, clear fluid, and gradual scab formation are typically part of the healing process.
Consult a specialist if symptoms do not improve or get worse.
Common Signs of Wound Infection
- Increasing pain rather than steady improvement
- Redness that spreads beyond the wound edges
- Warmth or swelling that continues to worsen
- Thick yellow, green, or foul-smelling drainage
- Fever, chills, or fatigue
- Red streaks extending away from the wound
If you notice these changes, you should schedule an appointment with a wound care specialist. Early evaluation and treatment can help prevent the infection from progressing and reduce the risk of complications.
What Should a Wound Look Like When Healing?
- Mild redness limited to the immediate edges
- Clear or light pink fluid
- Gradual reduction in swelling
- Wound edges that slowly pull together
- Decreasing tenderness over time
A healing wound should show gradual improvement rather than worsening. If you are unsure whether healing is progressing normally or infection is likely, get the wound checked.
When Should You See a Doctor for a Wound Infection?
Certain symptoms suggest that a wound infection may require medical treatment rather than continued home care. Recognizing these warning signs early can help prevent complications.
Signs of Wound Infection That Require Medical Treatment
A wound that looks stable at first can change quickly. Monitoring for worsening symptoms is an important part of safe wound care.
Seek medical evaluation if you notice:
- Redness that spreads beyond the wound edges
- Increasing pain instead of steady improvement
- Swelling or warmth that continues to worsen
- Thick yellow, green, or foul-smelling drainage
- Red streaks extending away from the wound
- Fever, chills, or unusual fatigue
These signs may indicate that bacteria are interfering with normal healing and that the infection is progressing rather than improving.
When to Call Your Wound Care Specialist Immediately
In addition to infection symptoms, certain situations warrant prompt evaluation. You should contact a wound care specialist promptly if you experience any of the following:
- A wound that has not improved after several days of appropriate care
- A deep, large, or gaping wound
- Bleeding that does not stop with steady pressure
- A wound caused by an animal bite, human bite, or contaminated object
- Any concerning wound if you have diabetes, vascular disease, or a weakened immune system
If you are in the Flint area and have concerns about a wound that is not healing as expected, Innovative Wound Care Specialists provides online wound self-assessment, advanced evaluation, and wound care treatments for both acute and chronic wounds.
Wound Infection FAQ
What does an infected wound look like?
An infected wound may appear increasingly red, swollen, or warm, with thick, yellow, green, or foul-smelling drainage. The surrounding skin may become tender, and redness may extend outward rather than remaining confined to the wound edges.
What are the five signs of wound infection?
Infections can present differently for each person. But generally, the five cardinal signs of infection are pus or foul-smelling discharge, increased pain or tenderness, warmth around the wound, spreading redness, and swelling. When a wound is infected, you may also have a fever, chills, or see red streaks extending from the wound.
What does pus from a wound mean?
Pus is a sign that the body is fighting an infection. Clear or light pink fluid can be normal during healing, but thick yellow, green, foul-smelling, cloudy, or increasingly heavy drainage should be evaluated by a healthcare professional.
When should I go to the ER for a wound infection?
You should seek emergency care if you develop a high fever, confusion, a rapid heart rate, severe spreading redness, red streaks traveling toward the body, or signs of systemic illness. These symptoms may indicate that the infection is spreading beyond the wound.
What happens if a wound infection goes untreated?
An untreated infected wound can delay wound healing, damage surrounding tissue, spread to deeper structures, and potentially even result in sepsis, amputation, or death. If you suspect your wound is infected, do not ignore it. Early evaluation reduces the risk of more serious complications.
Does diabetes increase the risk of wound infection?
Yes. Elevated blood sugar can impair circulation and the immune response, slowing wound healing and increasing the risk of infection. Individuals with diabetes should seek evaluation sooner if a wound does not improve or shows any signs of infection.
What is the fastest way to heal a wound at home?
The fastest way to support wound healing is consistent and proper skin care. Clean the wound using hand hygiene, keep it covered in a moist environment, change dressings regularly, and monitor for signs of infection.
How long should a wound take to start healing?
Wounds heal in stages. How quickly a wound heals depends on its type, size, and depth, and on your overall health. Minor wounds usually show gradual improvement within a few days. Chronic wounds, such as diabetic ulcers, venous ulcers, pressure injuries, burns, trauma wounds, or certain surgical wounds, may take significantly longer and often require specialized wound care treatment.
If a wound does not begin to improve or appears worse after several days of proper care, it should be evaluated.
Can your body fight a wound infection on its own?
In some cases, the immune system can manage minor bacterial contamination before a true infection develops. However, once clear signs of wound infection appear or symptoms worsen, medical evaluation is necessary to prevent complications and support proper healing.
What are the 4 C’s of wound care?
The 4 C’s of wound care are cleanse, control, cover, and check. This simple formula reinforces the core principles of proper wound management, reduces the risk of infection, and supports steady healing.
Your Partners in Safe Healing: Innovative Wound Care Specialists in Flint, Michigan
If you have concerns about a wound that is not improving and need to see a wound care specialist in Flint, Michigan, the multidisciplinary team at Innovative Wound Care is here to help. Our center brings together specialists in advanced wound care, vascular medicine, and infectious disease to address both the wound itself and the underlying factors affecting recovery.
We offer a variety of advanced wound care treatment options, including advanced wound dressings, debridement, negative pressure wound therapy, cellular or tissue-based products, compression therapy, and hyperbaric oxygen therapy.
If you have a wound that isn’t healing or might be infected, prompt evaluation and expert management can help ensure safe healing and reduce the risk of complications. Contact Innovative Wound Care Specialists to schedule an appointment or speak with a member of our care team.